132 billion pounds = money saved for the UK by unpaid carers.
6.5 million = number of carers in the UK.
6000 = number of people who become carers every day.
1 in 8 adults are unpaid carers for a family member or friend.
Carers UK call them ‘The Second NHS’.
Yet, do we or the Health Service truly value them? Listen to them? Include them? Give them a voice? Understand their concerns? Treat them as an ally? Respect their abilities and contributions? Answer their questions? Educate them? Empower them? Support them? Partner with them as well as we could? Sadly not.
In my experience and that of many other families of individuals with a mental illness, the power imbalance between the health care providers and the service users does not allow for an equitable relationship. Hence, denying the patient the best chances of recovery. There is national and local evidence that proves that carer engagement saves lives.

Triangulation of services is essential for best outcomes for patients and professionals. Risk averse practices may help reduce risk in the short term but may increase risk in the long term. A recovery approach to risk and development of a “life worth living” may have longer lasting benefits through rebuilding relationships, increasing service-users skills and confidence in collaboration with carers.
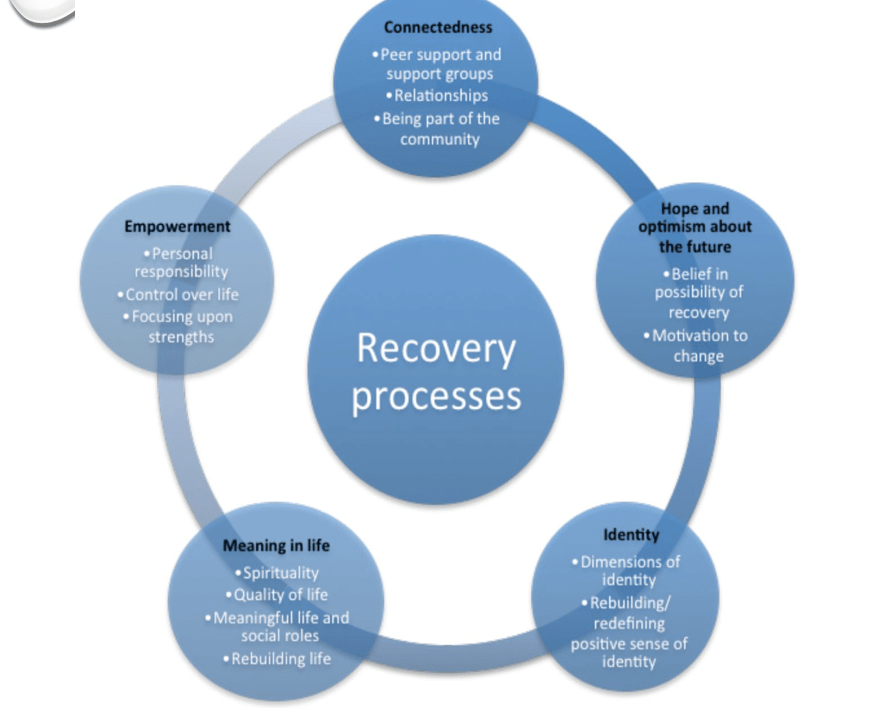
Norfolk and Suffolk Foundation Trust (NSFT) have developed a program called “Stepping Back Safely” up-skilling staff, carers and service-users. It is based on five main drivers of Recovery: CHIME
- Connection
- Hope
- Identity
- Meaning
- Empowerment
NSFT are offering free training in Stepping back Safely in July 2021 on-line. Having heard many stories where a life could have been saved only if there was a meaningful and effective communication between the three parts of the Triangle of Care, I think this training is most relevant and essential. I shall be taking it as I am sure it will deepen my understanding of the subject. If you or anyone you know might like a point of contact, here it is: catherine.phillips@nsft.nhs.uk